Breast Ultrasound Vs Mammogram: Key Differences Explained
February 18, 2026
Breast imaging is one of the most important tools in modern preventive medicine, yet it’s also one of the most misunderstood.
Many people hear terms like mammogram or ultrasound and immediately associate them with fear, discomfort, or uncertainty. This reaction is understandable—medical tests can feel intimidating, especially when they involve sensitive areas of the body. However, breast imaging exists for one primary reason: to provide clarity, not fear.
Breast imaging allows healthcare providers to see beneath the surface of breast tissue, identify subtle changes early, and guide patients toward timely care when it matters most. Rather than waiting for symptoms to appear, imaging gives clinicians a proactive window into breast health.
Understanding breast imaging is similar to understanding weather forecasts. You don’t need to be a meteorologist to appreciate why radar matters—you just need to know that it helps predict storms before they arrive.
In the same way, breast imaging helps detect potential health concerns before they escalate, offering reassurance when everything looks normal and decisive action when it doesn’t.
Why Breast Imaging Matters for Early Detection
Early detection can mean the difference between a simple treatment plan and a complex medical journey. Breast cancer, when identified early, is often highly treatable, with better outcomes, fewer invasive procedures, and higher long-term survival rates. Imaging makes this early detection possible by revealing abnormalities that are too small to feel during self-exams or routine physical checkups.
Many breast cancers develop silently. They may not cause pain, lumps, or visible changes in the early stages. Breast imaging fills this gap by acting as an early-warning system, allowing doctors to detect changes long before symptoms arise.
Think of breast imaging as a smoke detector rather than a fire extinguisher. Its role isn’t to respond after a crisis—it’s to alert you before the situation becomes serious. Regular imaging empowers patients to take a proactive stance rather than a reactive one, reducing both physical and emotional stress over time and providing peace of mind through consistent monitoring.
What Is a Mammogram?
A mammogram is a specialized X-ray exam designed specifically to evaluate breast tissue. It has long been considered the backbone of breast cancer screening programs worldwide and remains the most widely recommended screening tool for early detection.
Mammograms are particularly effective at identifying early-stage cancers that haven’t yet caused symptoms. They can reveal subtle abnormalities such as microcalcifications, asymmetries, or structural distortions that may indicate the earliest signs of cancer development.
Unlike standard X-rays, mammograms use very low radiation doses combined with advanced imaging technology. This balance allows radiologists to capture highly detailed images while keeping radiation exposure minimal and well within safety guidelines.
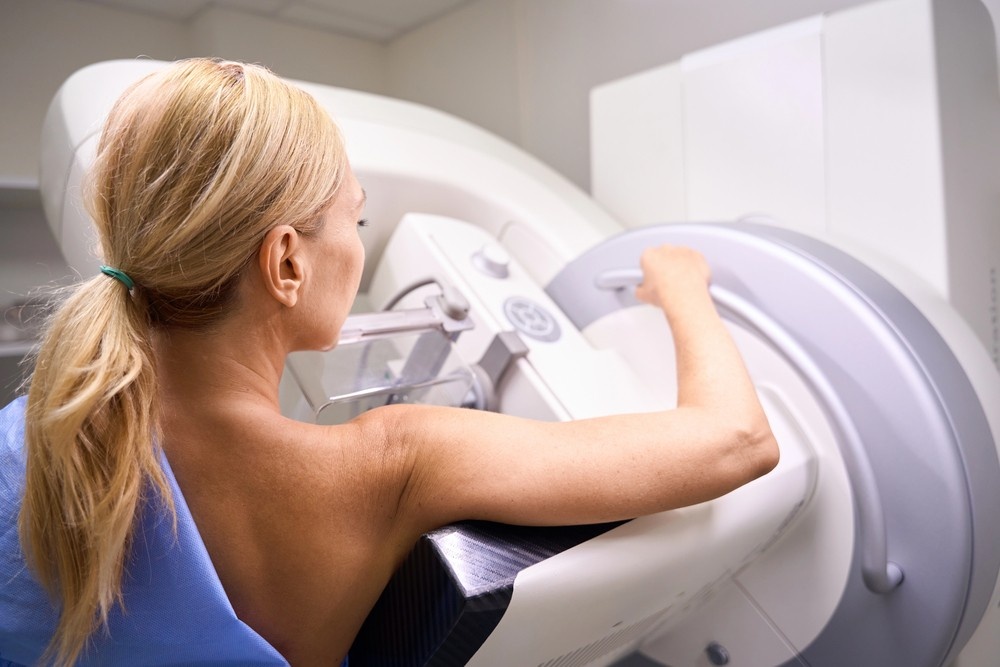
How Mammograms Work
During a mammogram, each breast is positioned on a flat surface and gently compressed between two plates. Compression may feel uncomfortable, but it plays a crucial role in image accuracy. It spreads breast tissue evenly, reduces overlapping structures, minimizes motion blur, and improves the visibility of small abnormalities.
The compression itself lasts only a few seconds per image. Most patients describe the sensation as pressure rather than pain. While the experience may be briefly uncomfortable, the benefit is long-lasting reassurance or early intervention if something unusual is detected.
Types of Mammograms
Mammograms are categorized based on purpose, ensuring that patients receive the right level of evaluation for their specific situation.
Screening Mammograms
Screening mammograms are routine exams performed on individuals without symptoms. Their primary goal is prevention through early detection. These exams are typically recommended annually or biennially, depending on age, risk factors, and clinical guidelines.
Over time, screening mammograms allow radiologists to compare current images with prior studies. This historical comparison improves accuracy by highlighting subtle changes that may develop gradually over the years.
Diagnostic Mammograms
Diagnostic mammograms are more detailed and are used when something unusual is detected, either during a screening mammogram or through physical symptoms such as a lump, pain, or nipple discharge.
These exams include additional views, magnification, and focused imaging of specific areas. Diagnostic mammograms help determine whether a finding is benign or requires further evaluation.
What Is a Breast Ultrasound?
A breast ultrasound is an imaging test that uses high-frequency sound waves to create detailed images of breast tissue. Unlike mammograms, ultrasounds do not use radiation, making them particularly useful for certain patients and clinical situations.
Breast ultrasound is often described as a problem-solving tool. It is commonly used to further evaluate areas that appear unclear on a mammogram or to assess findings discovered during a physical exam.
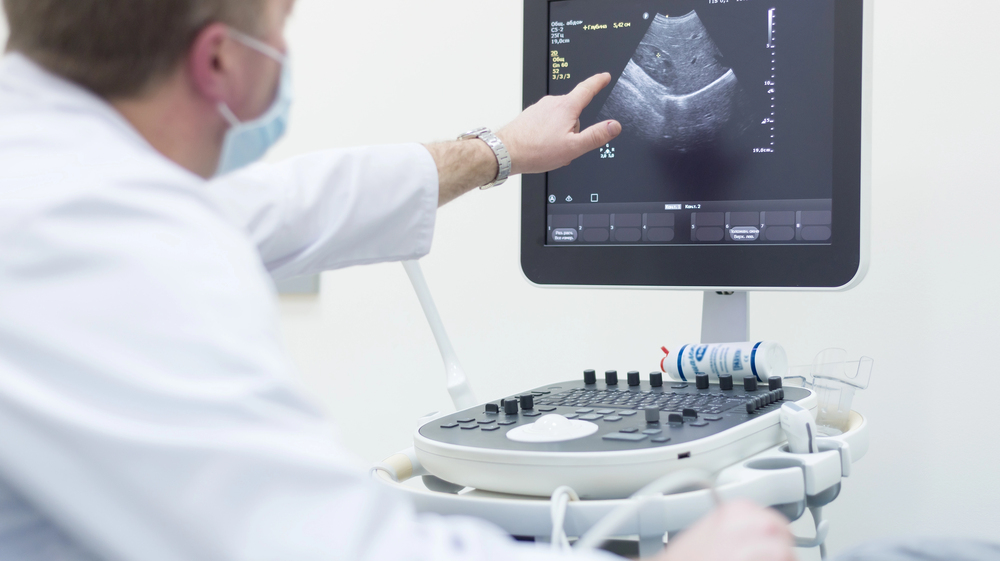
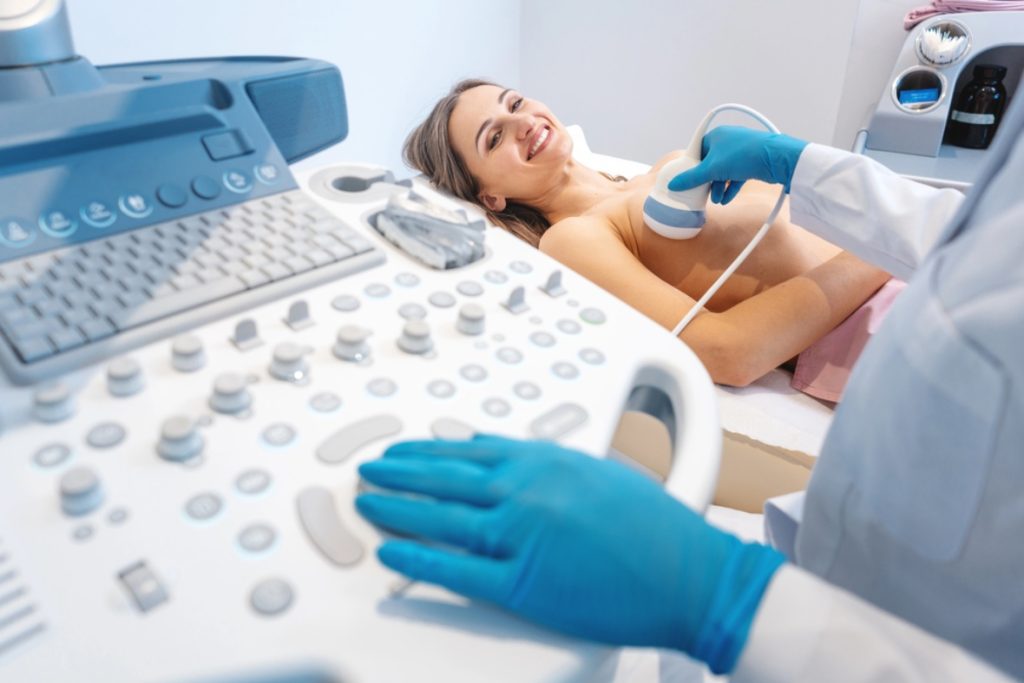
How Breast Ultrasound Works
During a breast ultrasound, a technologist applies a water-based gel to the skin and moves a handheld transducer across the breast. The transducer emits sound waves that travel into the tissue and bounce back as echoes.
These echoes are converted into real-time images displayed on a monitor. This live imaging allows clinicians to assess the shape, texture, and composition of breast structures, making it easier to determine whether a mass is solid or fluid-filled—an important distinction in breast diagnostics.
Types of Breast Ultrasound
Different ultrasound techniques are used depending on the clinical need and patient profile.
Handheld Ultrasound
Handheld ultrasound allows targeted examination of specific areas of concern. It is commonly used to investigate palpable lumps, localized pain, or abnormalities seen on mammograms.
Because the exam is interactive, radiologists can adjust angles, zoom in on suspicious areas, and evaluate tissue in real time, improving diagnostic confidence.
Automated Breast Ultrasound (ABUS)
ABUS scans the entire breast in a systematic and standardized manner. This method is especially beneficial for patients with dense breast tissue, where mammograms alone may be less effective.
ABUS creates a comprehensive image dataset that complements mammography and helps reduce the chance of missed findings in dense tissue.
Breast Ultrasound vs Mammogram: Core Differences
While both tests serve the same ultimate goal—early detection—their methods, strengths, and limitations differ significantly.
Imaging Technology Compared
Mammograms rely on X-rays to capture internal structures, making them excellent at detecting calcifications and subtle tissue distortions. Breast ultrasounds use sound waves, which are better suited for evaluating soft tissue differences and distinguishing cysts from solid masses.
In simple terms, mammograms function like a wide-angle lens, capturing the overall structure of the breast, while ultrasounds act like a zoom lens, providing close-up detail where needed.
Comfort and Patient Experience
Comfort is a common concern for patients. Mammograms involve compression, which some individuals find uncomfortable, particularly those with sensitive breasts. Ultrasounds, by contrast, are gentle and pressure-free.
That said, comfort should never outweigh diagnostic accuracy. The most effective imaging exam is the one that provides the clearest and most reliable information for your specific situation.
Accuracy and Effectiveness
Mammograms remain the most effective screening tool for the general population and are proven to reduce breast cancer mortality. Ultrasounds enhance detection in specific scenarios, such as dense breast tissue or follow-up evaluations, but are not designed to replace mammography as a standalone screening method.
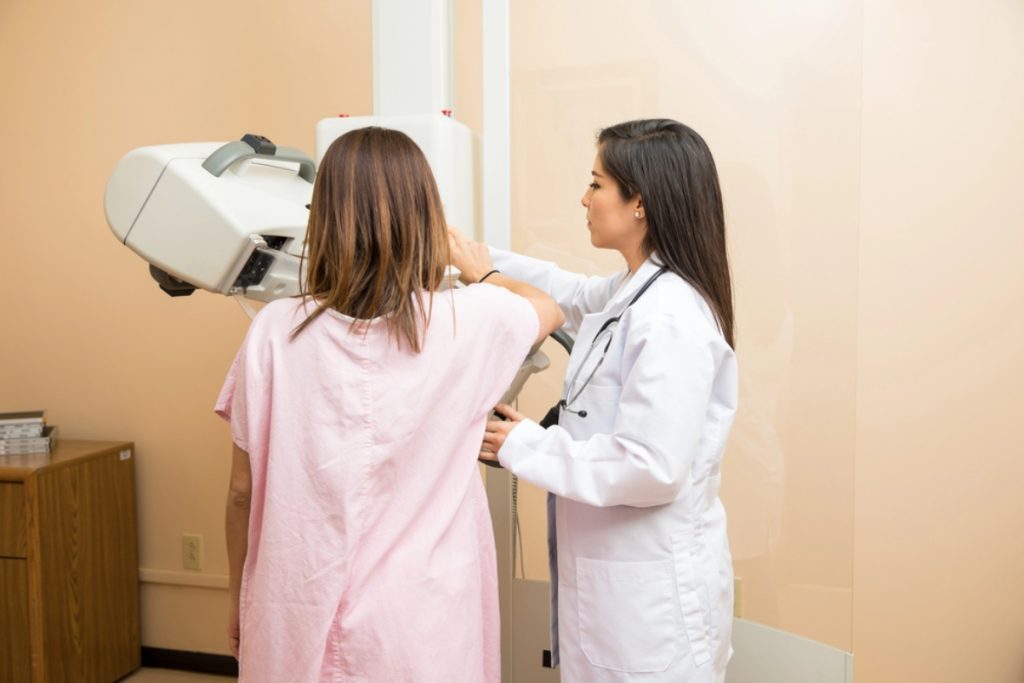
Which Test Is Right for You?
Choosing the right imaging exam is not a one-size-fits-all decision. Several personal and clinical factors influence which test—or combination of tests—is most appropriate.
Age-Based Recommendations
Age plays a significant role in screening recommendations. Mammograms are typically recommended starting at age 40 for average-risk individuals. Younger patients may begin imaging earlier if they have risk factors, and ultrasounds are often used first due to denser breast tissue in younger individuals.
Dense Breast Tissue Considerations
Dense breast tissue can make mammogram images harder to interpret because both dense tissue and tumors appear white on X-rays. Ultrasound adds an extra layer of visibility by highlighting differences in tissue composition, improving detection accuracy in dense breasts.
High-Risk Patients
Individuals with genetic mutations, strong family histories, prior breast cancer diagnoses, or other risk factors often require personalized imaging strategies. These may include more frequent screening and the use of multiple imaging modalities for thorough evaluation.
Benefits and Limitations of Mammograms
Mammograms offer several key benefits. They are fast, widely accessible, and supported by decades of clinical research. Mammograms are highly effective at detecting early-stage cancers before symptoms develop and allow for consistent long-term monitoring.
However, mammograms also have limitations. They may be less sensitive in dense breast tissue and involve minimal radiation exposure, though this exposure is extremely low and carefully regulated. False positives can occur, leading to additional imaging that ultimately proves benign.
Benefits and Limitations of Breast Ultrasound
Breast ultrasound is safe, comfortable, and radiation-free. It excels at evaluating specific areas of concern and distinguishing cysts from solid masses. Ultrasound is particularly useful for patients with dense breasts or those who cannot undergo mammography.
Its primary limitation is that it may miss certain early cancers, particularly those that present as microcalcifications. For this reason, ultrasound is typically used as a supplemental tool rather than a primary screening method.
Can You Have Both Tests?
Yes—and in many cases, combining both tests provides the most comprehensive assessment of breast health. Using mammography and ultrasound together allows radiologists to cross-reference findings, improving diagnostic confidence and reducing uncertainty.
This layered approach is especially valuable for patients with dense breast tissue or inconclusive findings. By leveraging the strengths of both imaging methods, clinicians can make more informed recommendations while minimizing unnecessary procedures.
Breast Imaging at NextGen Diagnostic Imaging near Mid West
Patients across the Mid West rely on NextGen Diagnostic Imaging for advanced breast imaging delivered with precision, compassion, and clinical expertise. The focus extends beyond technology alone to include clear communication, patient comfort, and accurate interpretation.
By combining advanced imaging equipment with experienced professionals, patients receive reliable results and guidance they can trust at every stage of their breast health journey.
Preparing for Your Breast Imaging Appointment
Preparation enhances both comfort and accuracy. Patients are advised to avoid deodorants, powders, perfumes, or lotions on the day of the exam, as these products can interfere with imaging results.
Wearing comfortable, two-piece clothing makes the process easier, and bringing prior imaging studies helps radiologists compare changes over time. Most importantly, asking questions and sharing relevant medical history ensures the imaging team can tailor the exam to your needs.
NextGen Diagnostic Imaging Serving the Mid West Community and Beyond in Houston
NextGen Diagnostic Imaging is dedicated to serving the diverse needs of the local community of Houston, including individuals residing in neighborhoods like Mid West. With its convenient location near landmarks such as the Briarmeadow Park and major intersections like Ann Arbor Dr and Beverly Hill St (coordinates: 29.73019301718039, -95.50934454470142), we offer breast ultrasound Houston services.
Get Breast Ultrasound at Mid West Now
Navigate from Mid West to NextGen Diagnostic Imaging Now
Conclusion
Breast imaging is not something to fear—it’s something to value. Understanding the differences between breast ultrasound and mammography allows you to take control of your health journey with confidence. These tools work best together, offering complementary insights that improve detection and decision-making.
By staying informed, following recommended screening guidelines, and choosing experienced imaging providers, you invest in clarity, prevention, and long-term peace of mind.
FAQs
1. Is breast ultrasound enough without a mammogram?
In most cases, no. Ultrasound is a supplemental tool and does not replace mammography for routine screening.
2. Does dense breast tissue increase cancer risk?
Dense breast tissue does not necessarily increase risk, but it can make detection more challenging, which is why additional imaging may be recommended.
3. Are mammograms safe long-term?
Yes. Mammograms use very low-dose radiation, and long-term studies support their safety and effectiveness.
4. How long does imaging take?
Most breast imaging exams are completed within 20–30 minutes, including preparation time.
5. Can imaging prevent breast cancer?
Imaging cannot prevent cancer, but it significantly improves early detection, which leads to better treatment outcomes.

NextGen Scan
Contact Us: We’re Here to Help!
We’d love to hear from you! Whether you have questions about our services, need more information on our diagnostic and pain management options, or would like to schedule an appointment, our friendly and professional team is here to assist you every step of the way. We are dedicated to providing you with the best care and support, and we are happy to address any concerns or inquiries you may have.